Opioids are a class of drugs naturally found in the opium poppy plant. Some prescription opioids are made from the plant directly, and others are made by scientists in labs using the same chemical structure. Opioids are often used as medicines because they contain chemicals that relax the body and can relieve pain.
Prescription opioids are used mostly to treat moderate to severe pain, though some opioids can be used to treat coughing and diarrhea. Opioids can also make people feel very relaxed and “high” – which is why they are sometimes used for non-medical reasons. This can be dangerous because opioids can be highly addictive, and overdoses and death are common. Heroin is one of the world’s most dangerous opioids, and is never used as a medicine in the United States.
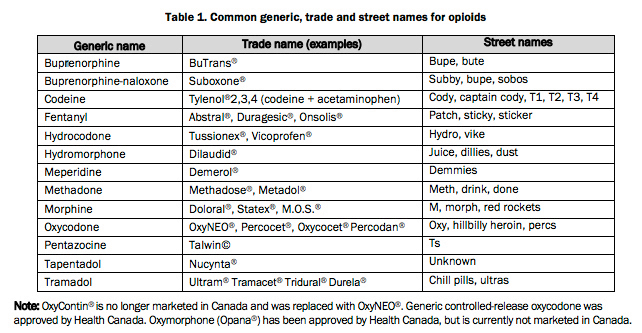
Popular slang terms for opioids include Oxy, Percs, and Vikes.
What are common prescription opioids?
- hydrocodone (Vicodin®) oxycodone (OxyContin®, Percocet®)
- oxymorphone (Opana®)
- fentanyl
- Hydromorphone (Dilaudid®)
- Morphine (Kadian®, M-Eslon®, MS-Contin®, Statex®, Avinza®
- Codeine (Tylenol No. 3®)
- Oxycodone (OxyNeo®, Percocet®)
- Tramadol (Ralivia®, Tridural®, Zytram®)
How do people misuse prescription opioids?
Prescription opioids used for pain relief are generally safe when taken for a short time and as prescribed by a doctor, but they can be misused. People misuse prescription opioids by:
- taking the medicine in a way or dose other than prescribed
- taking someone else’s prescription medicine
- taking the medicine for the effect it causes-to get high
When misusing a prescription opioid, a person can swallow the medicine in its normal form. Sometimes people crush pills or open capsules, dissolve the powder in water, and inject the liquid into a vein. Some also snort the powder.
How do prescription opioids affect the brain?
Opioids bind to and activate opioid receptors on cells located in many areas of the brain, spinal cord, and other organs in the body, especially those involved in feelings of pain and pleasure. When opioids attach to these receptors, they block pain signals sent from the brain to the body and release large amounts of dopamine throughout the body. This release can strongly reinforce the act of taking the drug, making the user want to repeat the experience.
Opioids have serious side effects and risks.
Over time, the body gets used to opioids and they stop working as well. To get the same relief, you need to take more and more. This is called “tolerance.” Higher doses can cause serious side effects:
- Nausea
- Vomiting
- Itching
- Constipation
- Not being able to urinate (empty your bladder)
- Slowed breathing, which can be deadly
- Confusion and mental disturbance
Opioid analgesics commonly cause drowsiness, dizziness, and respiratory depression. However, these side effects usually disappear with continued use. However, constipation, another common side effect, tends to persist. In addition, opioid use may lead to addiction or dependence. Other possible side effects of opioid analgesics include:
- Euphoria, dysphoria, agitation, seizures, hallucinations
- Lowered blood pressure and heart rate
- Muscular rigidity and contractions
- Nausea and vomiting
- Non-allergic itching
- Pupil constriction
- Sexual dysfunction
- Urinary retention
Opioids can be addictive. Long-term use of opioids can lead to “physical dependence” – if you stop using them abruptly, you will experience withdrawal symptoms, such as strong cravings, sweating, muscle aches and insomnia. People who take opioids long-term can become addicted, sometimes with dangerous results. In 2017, 4000 Canadians died from an opioid overdose.
Other pain treatments may work better and have fewer risks.
Pain medicine specialists say that usually you should try other treatments first:
- Over-the-counter medicines:
- Acetaminophen (Tylenol® and generic)
- Ibuprofen (Advil®, Motrin IB®, and generic)
- Naproxen (Aleve® and generic)
- Topical non-steroidal anti-inflammatory drugs (NSAIDs):
- Heat rubs
- Non-drug treatments:
- Exercise
- Physical therapy
- Spinal manipulation
- Massage therapy
- Acupuncture
- Cognitive behavioural therapy
- Injections (such as steroids)
- Other prescription drugs (ask about risks and side effects):
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Anti-seizure drugs
- Gabapentinoids
- Antidepressants
- Cannabinoids
When Might Opioids be Appropriate:
- You have cancer with severe pain: Opioids may be the right choice if pain is a bigger concern than the possibility of addiction and the need to keep increasing the dose.
- You just had surgery: If needed, you might be prescribed opioids, but they should not be used beyond the immediate period after surgery. This period is typically three days or less, and rarely more than seven days.
- You have chronic pain: Ask your health care provider about different options for managing pain, including non-opioid and non-drug alternatives before considering an opioid prescription. And ask about the risks and benefits among the options.
What should you do if your health care provider prescribes opioids?
Talk to your health care provider about the possible side effects and risks. Watch for side effects and signs of addiction. These include unusual moodiness or bursts of temper, cravings, and risk-taking.
Can I take prescription opioids if I’m pregnant?
If a woman uses prescription opioids when she’s pregnant, the baby could develop dependence and have withdrawal symptoms after birth. This is called neonatal abstinence syndrome, which can be treated with medicines. Use during pregnancy can also lead to miscarriage and low birth weight.
It can be difficult for a person with an opioid addiction to quit, but pregnant women who seek treatment have better outcomes than those who quit abruptly. Methadone and buprenorphine are the standard of care to treat opioid-dependent pregnant women. Methadone or buprenorphine maintenance combined with prenatal care and a comprehensive drug treatment program can improve many of the adverse outcomes associated with untreated opioid addiction. If a woman is unable to quit before becoming pregnant, treatment with methadone or buprenorphine during pregnancy improves the chances of having a healthier baby at birth.
In general, it is important to closely monitor women who are trying to quit drug use during pregnancy and to provide treatment as needed.
Can a person overdose on prescription opioids?
Yes, a person can overdose on prescription opioids. An opioid overdose occurs when a person uses enough of the drug to produce life-threatening symptoms or death. When people overdose on an opioid medication, their breathing often slows or stops. This can decrease the amount of oxygen that reaches the brain, which can result in coma, permanent brain damage, or death.
How can an opioid overdose be treated?
If you suspect someone has overdosed, the most important step to take is to call 911 so he or she can receive immediate medical attention. Once medical personnel arrive, they will administer naloxone. Naloxone is a medicine that can treat an opioid overdose when given right away. It works by rapidly binding to opioid receptors and blocking the effects of opioid drugs. Naloxone is available as an injectable (needle) solution, a hand-held auto-injector (EVZIO®), and a nasal spray (NARCAN® Nasal Spray).
Some states have passed laws that allow pharmacists to dispense naloxone without a personal prescription. This allows friends, family, and others in the community to use the auto-injector and nasal spray versions of naloxone to save someone who is overdosing.
Read more on our Naloxone webpage.
Can use of prescription opioids lead to addiction?
Yes, repeated misuse of prescription opioids can lead to a substance use disorder (SUD), a medical illness which ranges from mild to severe and from temporary to chronic. Addiction is the most severe form of an SUD. An SUD develops when continued misuse of the drug changes the brain and causes health problems and failure to meet responsibilities at work, school, or home.
People addicted to an opioid medication who stop using the drug can have severe withdrawal symptoms that begin as early as a few hours after the drug was last taken. These symptoms include:
- muscle and bone pain
- sleep problems
- diarrhea and vomiting
- cold flashes with goose bumps
- uncontrollable leg movements
- severe cravings
These symptoms can be extremely uncomfortable and are the reason many people find it so difficult to stop using opioids. There are medicines being developed to help with the withdrawal process, including lofexidine, a non-opioid medicine designed to reduce opioid withdrawal symptoms that was approved by the U.S. Food and Drug Administration (FDA) in 2018. The FDA has also approved sale of a device, NSS-2 Bridge, that can help ease withdrawal symptoms. The NSS-2 Bridge is a small electrical nerve stimulator placed behind the person’s ear, that can be used for up to five days during the acute withdrawal phase.
What type of treatment can people get for addiction to prescription opioids?
A range of treatments including medicines and behavioral therapies are effective in helping people with opioid addiction.
Two medicines, buprenorphine and methadone, work by binding to the same opioid receptors in the brain as the opioid medicines, reducing cravings and withdrawal symptoms. Another medicine, naltrexone, blocks opioid receptors and prevents opioid drugs from having an effect.
Behavioral therapies for addiction to prescription opioids help people modify their attitudes and behaviors related to drug use, increase healthy life skills, and persist with other forms of treatment, such as medication. Some examples include, cognitive behavioral therapy which helps modify the patient’s drug use expectations and behaviors, and also effectively manage triggers and stress. Multidimensional family therapy, developed for adolescents with drug use problems, addresses a range of personal and family influences on one’s drug use patterns and is designed to improve overall functioning. These behavioral treatment approaches have proven effective, especially when used along with medicines.
reference:
- choosingwiselycanada.org/patient-pamphlet-opioids/
- drugabuse.gov