 If you need to take opioids to control your pain, here are some ways to make sure you’re taking them as safely as possible. Opioid analgesia is indicated for the management of pain in patients where an opioid analgesic is appropriate. What, exactly, the term appropriate constitutes has been a recently contentious issue. Center for Disease Control and Prevention’s 2016 guidelines for prescribing opioids for chronic pain state that “clinicians should consider opioid therapy only if expected benefits for both pain and function will outweigh risks to the patient.
If you need to take opioids to control your pain, here are some ways to make sure you’re taking them as safely as possible. Opioid analgesia is indicated for the management of pain in patients where an opioid analgesic is appropriate. What, exactly, the term appropriate constitutes has been a recently contentious issue. Center for Disease Control and Prevention’s 2016 guidelines for prescribing opioids for chronic pain state that “clinicians should consider opioid therapy only if expected benefits for both pain and function will outweigh risks to the patient.When using opioids, it should be in combination with nonpharmacologic therapy and nonopioid pharmacologic therapy, as appropriate.” In the same guidelines, the CDC defines the indication of opioid use for acute pain, stating that “when opioids are used for acute pain, clinicians should prescribe the lowest effective dose of immediate-release opioids and should prescribe no greater quantity than needed for the expected duration of pain severe enough to require opioids. Three days or less will often be sufficient; more than seven days will rarely be needed.
Opioid analgesics – Commonly referred to as prescription opioids, medications that have been used to treat moderate to severe pain in some patients. Categories of opioids for mortality data include:
-
- Natural opioid analgesics, including morphine and codeine;
- Semi-synthetic opioid analgesics, including drugs such as oxycodone, hydrocodone, hydromorphone, and oxymorphone;
- Methadone, a synthetic opioid that can be prescribed for pain reduction or for use in MAT for opioid use disorder (OUD). For MAT, methadone is used under direct supervision of a healthcare provider;
- Synthetic opioid analgesics other than methadone, including drugs such as tramadol and fentanyl.
How Opioids Work ?
Opioid drugs bind to opioid receptors in the brain, spinal cord, and other areas of the body. They tell your brain you’re not in pain.
They are used to treat moderate to severe pain that may not respond well to other pain medications.
Opioids act both presynaptically and postsynaptically to produce an analgesic effect. Presynaptically, opioids block calcium channels on nociceptive afferent nerves to inhibit the release of neurotransmitters such as substance P and glutamate, which contribute to nociception. Postsynaptically, opioids open potassium channels, which hyperpolarize cell membranes, increasing the required action potential to generate nociceptive transmission. The mu, kappa, and delta-opioid receptors mediate analgesia spinally and supraspinally.
Also, some opioid agents can affect serotonin kinetics in the presence of other serotonergic agents. The proposed mechanism for this is through either weak serotonin reuptake inhibition and increased the release of intrasynaptic serotonin through inhibition of gamma-aminobutyric acidergic presynaptic inhibitory neuron on serotonin neurons. These opioids include tramadol, oxycodone, fentanyl, methadone, dextromethorphan, meperidine, codeine, and buprenorphine. These opioids have the potential to cause serotonin syndrome and should be used cautiously with other agents with serotonergic activity.
Opioids such as methadone also have activity at the N-methyl-D-aspartate (NMDA) receptor. Methadone binds to the NMDA receptor and antagonizes the effect of glutamate, which theoretically explains why methadone has efficacy in the treatment of neuropathic pain above other opioids.
Opioid analgesia is indicated for the management of pain in patients where an opioid analgesic is appropriate. What, exactly, the term appropriate constitutes has been a recently contentious issue. Center for Disease Control and Prevention’s 2016 guidelines for prescribing opioids for chronic pain state that “clinicians should consider opioid therapy only if expected benefits for both pain and function will outweigh risks to the patient.
When using opioids, it should be in combination with nonpharmacologic therapy and nonopioid pharmacologic therapy, as appropriate.” In the same guidelines, the CDC defines the indication of opioid use for acute pain, stating that “when opioids are used for acute pain, clinicians should prescribe the lowest effective dose of immediate-release opioids and should prescribe no greater quantity than needed for the expected duration of pain severe enough to require opioids. Three days or less will often be sufficient; more than seven days will rarely be needed.”
Forms of opioids
Opioid products come in many forms. They differ in how you take them as well as how long they take to start working and how long they keep working. Most of these forms can be taken without assistance. Others, such injectable forms, have to be given by a healthcare professional.
Immediate-release products start to work quickly after you take them, but they’re effective for shorter periods. Extended-release products release the drugs over longer periods. Products are generally considered immediate-release unless they’re labeled otherwise.
Immediate-release opioids are used to treat acute and chronic pain. Extended-release opioids are typically only used to treat chronic pain when immediate-release opioids are no longer enough.
If your doctor prescribes extended-release opioids to you, they may also give you immediate-release opioids to treat breakthrough pain, particularly for cancer pain or pain during end-of-life care.
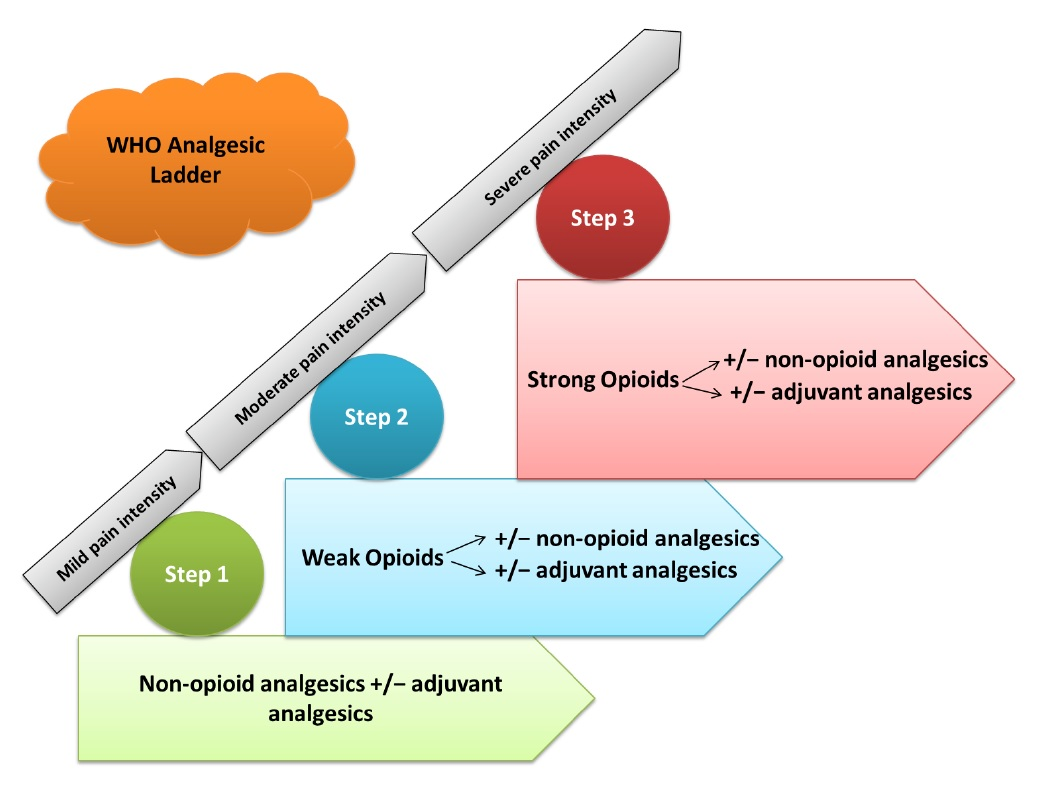
Opioid drugs include:
- Acetaminophen with codeine (Tylenol #2, #3, #4)
- Buprenorphine (Butrans)
- Fentanyl transdermal patches (Duragesic)
- Hydrocodone with acetaminophen (Lortab Elixir, Vicodin)
- Hydrocodone with ibuprofen (Vicoprofen)
- Hydrocodone (Zohydro)
- Hydromorphone (Exalgo)
- Meperidine (Demerol, Merpergan)
- Methadone (Dolophine)
- Morphine and morphine sustained release (MS-Contin, Avinza, Kadian)
- Oxycodone sustained release (OxyContin)
- Oxycodone with acetaminophen (Percocet)
- Oxycodone with aspirin (Percodan)
- Oxycodone with ibuprofen (Combunox)
- Oxymorphone (Opana, Opana ER)
- Pentazocine (Talwin,)
- Propoxyphene with aspirin, propoxyphene with acetaminophen
- Tapentadol (Nucynta, Nucynta ER)
- Tramadol, tramadol with acetaminophen (Ultram, Ultracet)
Table. Opioid Classification
| Classification | Examples |
| Strong Agonists |
|
| Mild to Moderate Agonists |
|
| Opioids with Mixed Receptor Actions |
|
Some relative contraindications to opioid analgesics include increased risk of prescription misuse. Several risk factors exist. These include:
-
Family or personal history of substance abuse
-
Young age
-
History of legal problems
-
Frequent contact with high-risk individuals or environments
-
History of previous problems with employers, family, and friends
-
History of risk-taking and thrill-seeking behavior
-
Smoking cigarettes and regularly using other substances that lead to dependence
-
History of major depression or anxiety
-
Multiple psychosocial stressors
-
History of childhood abuse
-
Previous drug and/or alcohol rehabilitation.
Also, other opioid-specific toxicities exist, which may preclude their use in specific populations. For example, as mentioned above, opioids with serotonergic activity have the potential to lower the seizure threshold, and should, therefore, be used cautiously or avoided entirely in patients with a history of seizure disorder to avoid causing or worsening seizures. Opioids such as methadone, which have the potential to prolong QTc interval should be used cautiously or avoided entirely in patients with Long QT syndrome.
Opioid Side Effects
One of the reasons why your doctor needs to manage pain medications so closely is that they can cause side effects, such as:
- Constipation
- Drowsiness
- Nausea and vomiting
The drugs lubiprostone (Amitiza), methylnaltrexone (Relistor), naldemedine (Symproic), and naloxegol (Movantik) are approved to treat constipation due to opioid use in those with chronic pain.
Opioids can be dangerous if you take them with alcohol, or with certain drugs such as:
- Some antidepressants and anxiety medications (particularly benzodiazepines such as alprazolam, ativan and clonazpam)
- Some antibiotics
- Sleeping pills
Make sure your doctor knows all of the other medicines you’re taking. That includes:
- Prescription drugs
- Over-the-counter drugs
- Herbal supplements
Opioid Tolerance and Addiction
After taking opioid pain medication for a while, you might find that you need more and more of the drug to achieve the same effect in easing pain. This is called tolerance. It’s not the same as addiction, which involves a compulsive use of a drug.
When you use opioid medication over an extended period of time, you can have dependence. This can happen when your body becomes so used to the drug that if you abruptly stop taking it, you get withdrawal symptoms such as:
- Diarrhea, nausea, and vomiting
- Muscle pain
- Anxiety
- Irritability
You can also get a serious addiction to opioid pain medications. People who are addicted compulsively seek out the pain medications. Their behavior usually leads to negative consequences in their personal lives or workplace. They might take someone else’s pills or buy them off the street, which is especially dangerous since those drugs are often laced with lethal amounts of fentanyl. Learn more about what can happen when opioid addiction goes untreated.
If you are having a problem with addiction, you need to see your doctor or an addiction specialist.
Commonly Abused Narcotics & Opioids
Below is a brief list of some of the more widely-known narcotics and opioids drugs:
- Opium
- Heroin
- Codeine
- Oxycodone
- Hydrocodone
- Tramadol
- Morphine
- Hydromorphone
- Fentanyl
- Carfentanil
The United States is in the midst of an opioid epidemic. The American Society of Addiction Medicine (ASAM) indicates that close to 3 million people battled opioid addiction (to either heroin or prescription painkillers) in 2015. More than 60 percent of the record-high overdose deaths in 2015 involved an opioid drug, and 91 people in the US die from an opioid overdose daily, the Centers for Disease Control and Prevention (CDC) reports. Also in 2015, roughly 300 million prescriptions were dispensed for narcotic pain medications around the world, and Americans consumed 80 percent of them.
Opioid abuse, addiction, and overdose are considered serious public health concerns in the United States. Here we’ll provide more detail about some of the more commonly discussed prescription painkillers and illicit narcotic drugs.
Should You Take Opioid Pain Medications?
Opioids can make a dramatic difference to people with moderate to severe pain, but they aren’t always the right choice. Discuss the necessity of using them with your doctor. If you take them, follow your doctor’s instructions carefully. If your pain isn’t related to cancer, talk with your doctor regularly about whether you need to keep taking opioids. If you need to continue taking them, lowering the dose or changing the type of opioid may help prevent problems.
Opioids vs non-Opioids
Non-opioid medications may be beneficial in helping to control chronic pain. Some examples of non-opioid pain medications include over the counter medications such as Tylenol (acetaminophen), Motrin (ibuprofen), and Aleve (naproxen). Some prescription medications may also be used to manage pain. Neurontin (gabapentin) is often prescribed to manage nerve pain. Corticosteroids may be used to decrease pain caused by inflammation, and some types of antidepressants may also be effective in treating chronic pain. Sometimes, your doctor may recommend a topical pain medication such as lidocaine or capsaicin.
It is important to discuss the use of these medications with your doctor as they may have dangerous interactions with other prescription medications or cause dangerous side effects for some people.
Opioids are medications used to relieve severe pain. They reduce the intensity of pain signals from your body and change how your brain perceives pain. Typically, opioids are prescribed to people who are injured, are recovering from surgery, or are suffering from chronic pain.
Toxicity of Opioids
Opioids can result in fatal overdose through respiratory depression, especially when combined with other sedatives such as alcohol and benzodiazepines. Patients with altered mental status, depressed respiration, and constricted pupils should be suspected of presenting with an acute opioid-related overdose, which can be fatal if untreated.
Overdose is reversible by agents such as naloxone, which can be given intravenously, intramuscularly, or intranasally. Naloxone is a centrally-acting pure opioid antagonist with a high affinity at mu-opioid receptors, which quickly counteracts opioid action. At normal doses in the absence of opioid agonists, it has virtually no pharmacologic activity.
Naloxone can be given in small, repeated doses and titrated to a desirable response. Naloxone is active for 30 to 60 minutes before being deactivated by the liver, which may make it necessary to repeat the administration of naloxone over an extended timeframe for an overdose of long-acting opioid analgesic dosage forms.
Other opioid-specific toxicities that are worth mentioning also exist. For example, methadone carries a risk of QTc prolongation and, in some cases, torsades de pointes. Furthermore, opioids that have a serotonergic action, for example, tramadol, can cause seizures and serotonin syndrome.
Steps for Safe Use of Opioids
Using opioids, even for short periods, can lead to addiction and overdose. There are a few steps you can take to use opioids safely:
- Tell your doctor about any history of substance misuse so they can carefully monitor you during treatment with opioids.
- Follow the directions on your prescription. Taking too much or taking a dose incorrectly (such as crushing pills before taking them) can lead to more side effects, including difficulty breathing and overdose.
- Talk to your doctor about what substances you should avoid while taking an opioid. Mixing opioids with alcohol, antihistamines (such as diphenhydramine), benzodiazepines (such as Xanax or Valium), muscle relaxants (such as Soma or Flexeril), or sleep aids (such as Ambien or Lunesta) can increase your risk for dangerously slowed breathing.
- Store your medication safely and out of reach of children. If you have any unused opioid pills, take them to a community drug take-back program.
Takeaway
There are many opioids available to treat acute and chronic pain as well as more specific conditions. Some products may be more appropriate for you, so talk with your doctor to make sure they know about factors that could influence the treatment they recommend for you.
After starting an opioid product, make sure to see your doctor regularly and talk about any side effects or concerns you have. Because dependence can develop over time, also talk with your doctor about what to do if you feel it happening to you.
If you want to stop your opioid therapy, your doctor can work with you on a plan to safely stop taking them.
What is the difference between “tolerance,” “dependence,” and “addiction”?
Opioid tolerance occurs when a person using opioids begins to experience a reduced response to medication, requiring more opioids to experience the same effect.
Opioid dependence occurs when the body adjusts its normal functioning around regular opioid use. Unpleasant physical symptoms occur when medication is stopped.
Opioid addiction (Opioid use disorder (OUD)) occurs when attempts to cut down or control use are unsuccessful or when use results in social problems and a failure to fulfill obligations at work, school, and home. Opioid addiction often comes after the person has developed opioid tolerance and dependence, making it physically challenging to stop opioid use and increasing the risk of withdrawal.